Superbugs could lower your life expectancy by nearly 2 years, report says. What to know about antimicrobial resistance
As one public health threat takes a bow, another takes center stage. Less than a year after the end of the federal COVID-19 Public Health Emergency, a group of international political, public health, and biomedical leaders warns of another menace to human life that could also trigger economic loss.
Antimicrobial resistance (AMR)—which occurs when certain germs survive the drugs engineered to eradicate them—is on track to lower global life expectancy by an average 1.8 years by 2035, according to a new report from the Global Leaders Group (GLG) on Antimicrobial Resistance. For some low- and middle-income countries, life expectancy could fall by as much as 2.5 years.
AMR is also poised to have “a catastrophic effect on the global economy,” the report says, with projected losses totaling $855 billion annually until 2035. About $412 billion accounts for the health care costs of treating resistant bacterial infections; the other $443 billion represents productivity losses and lower workforce participation due to increased morbidity and mortality.
Released earlier this month, the GLG on AMR report calls on member states of the United Nations to aggressively mitigate the global health hazard. This includes, per an accompanying news release, securing funding “to tackle the dwindling research and development pipeline for new antibiotics.” Eight years after the first UN high-level meeting on AMR, the UN General Assembly in September will convene for its second meeting.
“We have the tools to mitigate the AMR crisis and these data point to a devastating future if we do not take bolder action now,” Mia Amor Mottley, prime minister of Barbados and chair of the GLG on AMR, said in the news release. “That is why the Global Leaders Group is making recommendations and proposing targets to drive a robust global response to AMR and save millions of lives.”
Why is AMR a global public health threat?
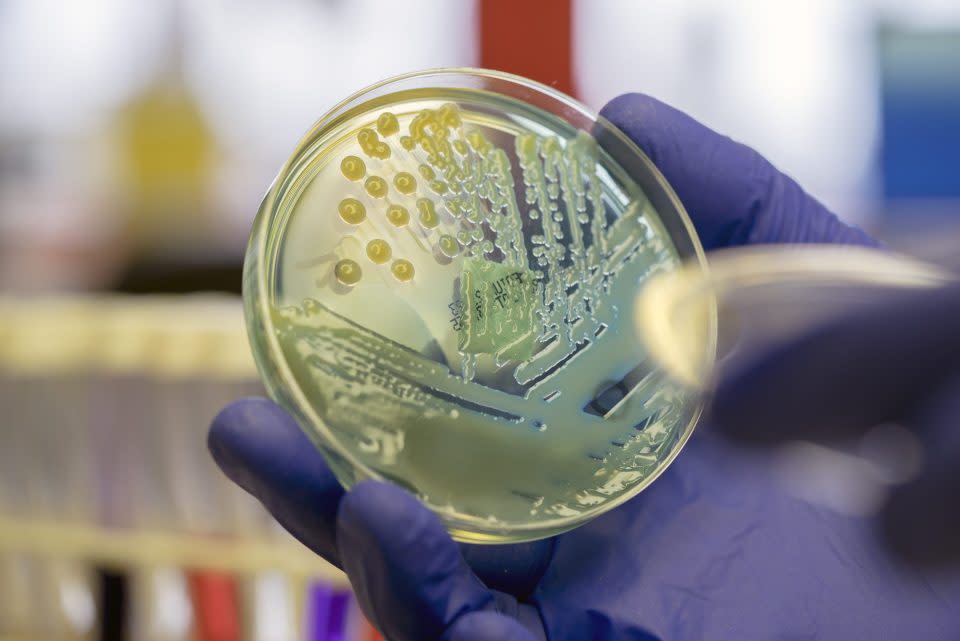
Fungi, parasites, viruses, and bacteria can cause infections in plants, animals, and humans. They can also evolve to a point where they no longer respond to antimicrobial medicines: antifungals, antiparasitics, antivirals, and antibiotics. The term “superbugs” refers to such microorganisms that develop AMR, according to the World Health Organization (WHO).
“This is made worse when people overprescribe antibiotics,” Jamie Alan, PharmD, PhD, an associate professor in the Department of Pharmacology and Toxicology at Michigan State University, tells Fortune. “Many times, people don’t actually need an antibiotic.”
If you have an ear infection, for example, it could be viral or bacterial, Alan explains. You feel awful, you’ve taken the time to go to the doctor’s office, and you expect to walk away with an antibiotic. If you do have a bacterial infection, chances are you’re already on your way to recovery by the time you seek medical attention, she says. If your infection is viral, antibiotics will not only not treat your illness but also give your bug an opportunity to mutate. You can then spread the mutated bug to others.
“That ultimately culminates in an effect where we have these superbugs that are resistant to many antibiotics,” Alan says. “When people become infected with those bugs, they have a higher chance of death, simply because now many of our antibiotics will not work.”
AMR contributed to 4.95 million deaths in 2019 alone, according to an analysis published in the medical journal The Lancet. Of those, AMR was directly responsible for 1.27 million. The WHO identified AMR as a top global public health and development threat, and the GLG on AMR proposed reducing global deaths by 10% by 2030.
While the scope of the problem may feel insurmountable, it must be treated as the worldwide quandary it is, says Dr. William Schaffner, a professor in the Division of Infectious Diseases at Vanderbilt University Medical Center.
“We are a global village. What’s over there can be over here in no time at all,” Schaffner tells Fortune. “If [people] get sick here in the United States and they’ve come from abroad and they’ve brought those antibiotic-resistant bacteria with them, then we have to treat them here. And this speaks to our own citizens who travel abroad.”
He adds, “We have to think about this as both a local problem and a global problem.”
Drugmakers need incentives to develop new antimicrobials
Practicing antibiotic stewardship, which entails prescribing fewer antibiotics, is the first step in curbing AMR, Schaffner says: “The less we use, the more the bacteria will remain susceptible to the antibiotics that we currently have.”
Overprescription extends to pediatric patients, too, Alan stresses. As a parent herself, she tells Fortune she understands the instinct to seek medicine for your sick child, but that antibiotics aren’t appropriate for every ailment.
The pharmaceutical industry also has a critical role to play in the solution. Developing new antibiotics is more complex and expensive than ever, Schaffner says. In addition, demand for antibiotics is fleeting; you take them here and there throughout your life, as opposed to, say, blood pressure medication you take for years on end. Bottom line, pharmaceutical companies are presented with a hefty investment that would likely result in little return.
Further dampening the incentive is a counterintuitive business model, Schaffner explains. “I can think of no other circumstances in all of commerce [where] a new product comes out—a new antibiotic in this circumstance—and the first thing that the infectious disease community says is, ‘Don’t use it. Save it. Use it only if the others don’t work.’”
That’s because even if a new antibiotic were to hit the market tomorrow, it would need to be prescribed sparingly to ensure it’s able to fight off bacteria for years to come, Schaffner says. As such, the GLG on AMR report outlines how public and private funds may be used to incentivize pharmaceutical companies and drive drug development.
In the U.S., the proposed Pioneering Antimicrobial Subscriptions To End Upsurging Resistance (PASTEUR) Act of 2023 calls for the establishment of the Committee on Critical Need Antimicrobials. The PASTEUR Act would appropriate $6 billion toward fighting AMR and entail subscription contracts with drug developers. Despite having bipartisan support, however, the bill remains stalled in the Senate.
Another goal of the GLG on AMR is to reduce the number of antimicrobials used in agriculture by 30–50% by 2030. Implementing all of the group’s proposed global interventions would cost about $46 billion annually. Yet every dollar spent by 2050 would garner an estimated return of up to $13.
Until more concrete action is taken, keeping AMR under control with the antibiotics currently at our disposal is a group effort, Schaffner says.
“Much of it is on us—the general public, the medical profession, the veterinarians, and the agriculture industry—to work together to make sure that these antibiotics will continue to be active in ways that we can treat people who are sick and treat animals that are sick,” he says.
For more on antimicrobial resistance:
This story was originally featured on Fortune.com
